Topic Refresher: Hypertension Treatment Guidelines
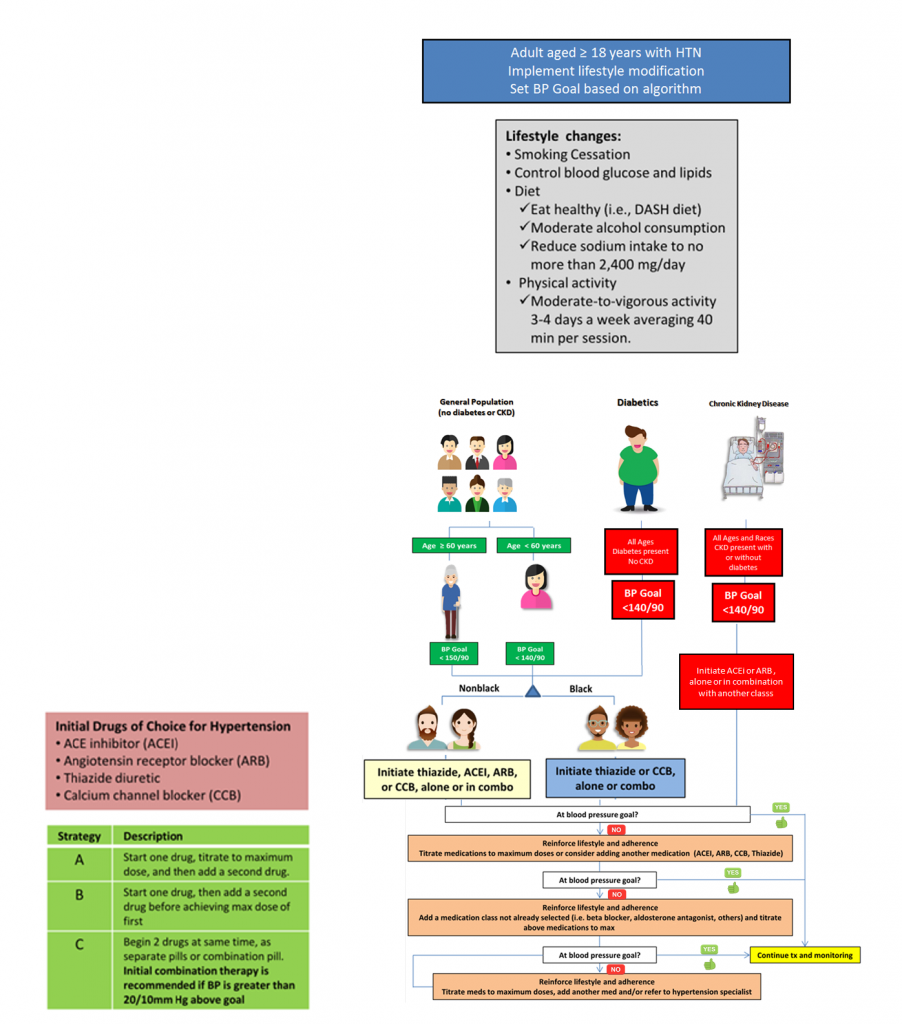
The Eighth Joint National Committee (JNC 8) recently released evidence-based recommendations on treatment thresholds, goals, and medications in the management of hypertension in adults.
Always start with lifestyle modification even if drug therapy is also needed:
- A diet rich in fruits, vegetables, and low-fat dairy foods and low in saturated and total fats (DASH diet) has been shown to lower blood pressure.
- Weight loss (to body mass index [BMI] of 18.5—24.9)
- Salt restriction (<6g sodium chloride or <2.5 g sodium)
- Limited alcohol use (12 oz of beer, 5 oz of wine, 1.5 oz of 80-proof whiskey)
- Stress management
- Smoking cessation
- Regular aerobic exercise (3-4 days/week averaging 40 minutes per session)
In the general population of adults 60 years and older, pharmacologic treatment should be initiated when the systolic pressure is 150 mmHg or higher, or when the diastolic pressure is 90 mmHg or higher. Patients should be treated to a target systolic pressure of less than 150 mmHg and a target diastolic pressure of less than 90 mmHg. Treatment does not need to be adjusted if it results in a systolic pressure lower than 140 mmHg, as long as it is not associated with adverse effects on health or quality of life.
In the general population younger than 60 years, pharmacologic treatment should be initiated when the systolic pressure is 140 mmHg or higher, or when the diastolic pressure is 90 mmHg or higher. The target systolic pressure in this population is less than 140 mmHg, and the target diastolic pressure is less than 90 mmHg.
Hypertension in Patients with CKD or Diabetes: For persons 18 years or older with chronic kidney disease (CKD) or diabetes mellitus, the treatment threshold and target blood pressures are the same as those for the general population younger than 60 years (i.e., threshold systolic pressure of 140 mmHg or threshold diastolic pressure of 90 mmHg; target systolic pressure of less than 140 mmHg; target diastolic pressure of less than 90 mmHg). There is no evidence that treating patients with CKD to a lower blood pressure goal slows the progression of the disease. Similarly, there is no evidence from randomized controlled trials showing that treatment to a systolic pressure of less than 140 mmHg improves health outcomes in adults with diabetes and hypertension.
Initial Drugs of Choice for Hypertension include:
- ACE inhibitor (ACEI)
- Angiotensin receptor blocker (ARB)
- Thiazide diuretic
- Calcium channel blocker (CCB)
- Note: Beta Blockers are no longer recommended as first line agents
Pharmacologic Treatment In the general nonblack population, including those with diabetes, initial anti- hypertensive treatment should include a thiazide diuretic, calcium channel blocker, angiotensin-converting enzyme (ACE) inhibitor, or angiotensin receptor blocker (ARB). In the general black population, including those with diabetes, initial treatment should include a thiazide diuretic or calcium channel blocker. If the target blood pressure is not reached within one month after initiating therapy, the dosage of the initial medication should be increased or a second medication should be added (thiazide diuretic, calcium channel blocker, ACE inhibitor, or ARB; do not combine an ACE inhibitor with an ARB). Blood pressure should be monitored and the treatment regimen adjusted until the target blood pressure is reached. A third drug should be added if necessary; however, if the target blood pressure cannot be achieved using only the drug classes listed above, antihypertensive drugs from other classes can be used (e.g., beta blockers, aldosterone antagonists
Adults with CKD and hypertension should receive an ACE inhibitor or ARB as initial or add-on therapy, based on moderate evidence that these medications improve kidney-related outcomes in these patients.